The word ‘participatory’ has been used in engagement and research to cover a wide variety of activities that involve any level of community involvement. But how should we really define participatory? Is it ok for activities that involve a very small amount of direct involvement to be called participatory? Praxis Institute for Participatory Practices, based in Delhi, India, argue that true participation means involving community members in every stage of any governance process, from research initiation – which should be based on priorities set by the community - to policy decision making. Pradeep Narayanan, Director of Research and Capacity Building at Praxis presented their work at the 2018 Wellcome International Engagement Workshop, explaining how engagement practitioners can learn from their Participatory, Action, Research principles to make their work truly participatory at every stage.
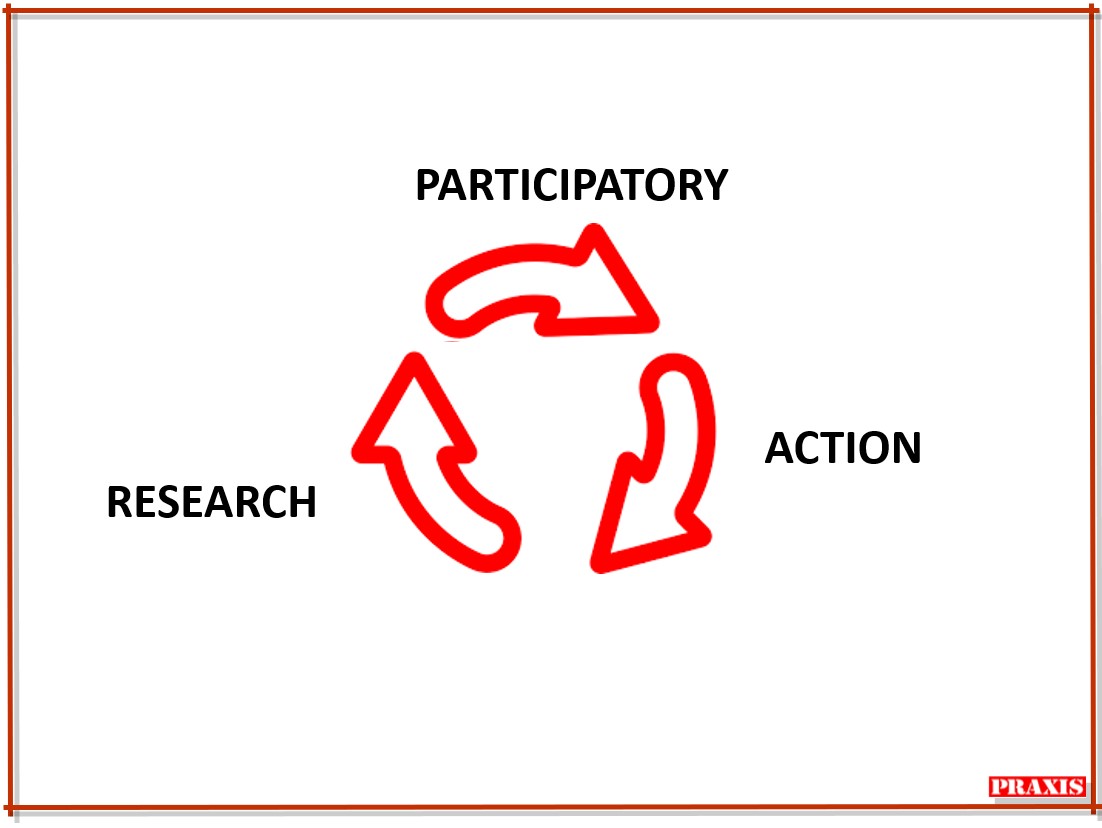
Image: The Participatory-Action-Research cycle | Praxis
As an engagement practitioner, how do you usually define the problem you are aiming to solve? Praxis suggested that when this problem is defined by traditional research and taken on by the engagement community, we are ‘pre-fining’ the problem; how can we be sure that this is truly a problem felt strongly by the community we are trying to serve, and that there are not other, more pressing problems we should be working to solve first?
This creates challenging questions for those working in engagement: what is our responsibility to enforce the health agenda decided by top-down processes? How do we balance this with a more progressive, community-led agenda, and what do you do when the two may not align? Can and should you influence the community’s knowledge and understanding of a subject to shift their agenda?
Praxis argue that it is expected and normal for researchers to have an agenda – everybody working within society has one. However, the important thing is to not be dominant in interactions; if you are, you will only reach those who already agree with you and you won’t have the opportunity to learn from those with different experiences. Behaving like this won’t prevent research from happening – after all, it is the way research has been done for centuries! But by not being truly participatory, any research outputs may not align with the needs of the community, making them difficult to implement and potentially damaging from the community’s perspective. Praxis presents Participatory Action Research (PAR) as the way to avoid these struggles.
What is Participatory Action Research not?
In many ways, it is easier to explain Participatory Action Research by explaining what it is not:
- Research with no participatory or inclusive engagement activities at all.
- Extractive participatory research – where researchers use a community to get data and participants for their research, but offer nothing else.
- A project that begins as researcher-led, then shifts to community-led in its later stages – can it ever actually be truly community-led if the community wasn’t involved at the start?
- Research that begins as participatory, then shifts to action research partway through – action research must be integrated from the beginning and must continually shape the process.
What is it?
Praxis see the PAR method as a cycle, where participation feeds into action, which feeds into research, which then leads to participation with the results, which then feeds further action, which produces more research, and so on. In PAR participation should be present in defining purpose; in research design, data collection, analysis, dissemination and use.
How is it done?
1. Mapping and Scoping
The first step is to understand the community, not as a homogenous mass, but understand the power dynamics, what is already being done and who you need to influence for change to occur. You will only ever be able to bring a small sample of people to the table, they won’t always be “representative” and you will be working with deep seated power dynamics.
2. What Evidence is Needed
What evidence is needed by the community? Decide in community meetings what data is relevant and what tools are needed to collect it. Also be aware of capacity issues for the community to collect and analyse data.
3. Tools
Develop tools with community to collect data.
4. Data collection and Analysis
Be flexible about what data looks like, it won’t look like data researchers are used to seeing. Think about methods to synthetize knowledge for and with the community.
5. Dissemination and Communication
Any interventions resulting from the PAR process need to be community led. They also need to be confident in influencing any policy and action. As facilitator, you may need to harmonise if people in “power” in the research or influence roles decide on different intervention than the community. Or, if different sections of the community disagree.
6. Evaluation and Learning with Communities
Ensure there is resource to continue relationships where possible.
Key Components and Benefits
Relaying the problem onto the community and being merely a tool for them to conceive of a solution ensures ownership and means less need for incentivisation. In PAR, the action should be led by the community.
Challenges
If the action is led by the community, we need to adopt a do no harm approach to ensure there are not negative impacts. The session included extensive debate on the practicalities and ethics of the approach, some of these challenges are captured below.
Three levels of research buy in are required to absorb PAR into biomedical research
Researcher (personal) – attitude
Researcher (professional) – data and methods
Institutional - supportive environment
How to we build relationships and break hierarchy between research and community?
1. Locate yourself on their level, allow them to present their knowledge first. Do not start with your own expertise, as it will become hierarchical and they will just listen.
2. Move from researcher/community questions to a group asking questions of each other. Respect the silence as a researcher or engagement practitioner, the community members will fill it with their own experience if given the time to do so.
3. Democratise the process so others get a chance to speak. As the conversation progresses, write comments down for all to see. If you want to ensure you are capturing stories correctly, or not misinterpreting points (which can be disempowering) you can validate each point as you write, but balance this with breaking up process.
4. Allow people to change their opinion and take back information if they want to. A survey misses this as it captures one point of time, but PAR reflects evolving mindsets.
Who is best placed to run PAR?
A good listener. There are pros and cons to different people running PAR.
Biomedical Researchers may not always have the skills, or may carry bias, but by being present the viewpoints of the community sink in much better.
Community engagement practitioners often have the skills but don’t always have buy in at senior level in research institutions.
Community members, if they are bought in, can self-organise and run focus groups and research themselves.
Issues to consider in data collection
- You will hear multiple differing voices and research has to choose one or synthesise
- There are existing power relationship
- Certain methods may be exclusionary (access, disability)
- Be clear what you want – transaction or relationship (You give me X e.g data, I’ll give you Y e.g government change, or analysis). If you only want to explore one research area, will you get pulled into wider areas that are not relevant?
Ethics
Consent is a difficult issue for PAR. Consent letters predominantly protect the institution, not the community. Consent can dis-empower as you cannot take back consent and own your own decisions. Who is able to be the gateskeeper to the community to sign consent? And what does ethics actually mean to that community? The red line may be different and needs to be discussed. Community Based Ethical Review Committees can be helpful.
Payments and Incentives
Payment can kill off the research that cannot afford to pay community and it can be argued that the community don’t own problem when they are paid for the process. But, the power imbalance is strengthened by lack of payment as, inevitably, someone is being paid. What funding might the community apply for to support their contributitions?
Timescales
How do you account for the timescale of impact? Often if the problem is solved, it won’t be an immediate pay-off for the community, it could be many years or decades away. You can focus on the greater good vs immediate family and friends but is this what people have capacity to care about when living in difficult circumstances?
Other Barriers
How do you manage expectations or the community naturally seeing the researcher as a problem solver and defaulting to them?
How to you solve wider problems that arise in PAR beyond those related to your research? (e.g literacy, income generation)
Researchers can be scared to loose funding if PAR shows they need to change course.
Making Space for PAR
There are several things that could make PAR more realistic:
Space within biomedical grants to flex in response to PAR and/or a requirement to do so.
Institutions using other parts of it’s machine to help solve problems that arise outside of the researcher remit.
Identify where you need community empowerment for research and impact to succeed and funnel PAR in those areas.
The process is important to disrupt power relationship – even if nothing else achieved.
---
The content on this page forms part of the online report for the 2018 International Engagement Workshop “Taking it to the Next Level: How can we generate leadership and develop practice in engagement?". To learn more about the workshop, access the rest of the report and browse the video presentations, discussion summaries, and tools, visit the workshop page.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Please Sign in (or Register) to view further.